
HERNIA Treatments
Reviewed By: Dr. Paul Szotek
Will a hernia heal on its own?
Our bodies have remarkable regenerative healing capabilities, but sometimes they need a little help.
While watchful waiting may be a viable option for a limited period of time, hernias typically require a surgical procedure to fully repair the defect and reduce the risk of a trip to the emergency room.1

I have this bulge, but no pain. Is there a way to hide it?
For decades, properly fitted support garments like hernia belts (truss) or briefs have been effectively used to reduce the visible appearance of a hernia. However, this non-surgical option is a short-term solution and will require a consultation with your doctor to determine proper fit and assessment of your condition.

Hernia Surgery
A relatively routine procedure with over one million performed each year in the US2. Hernias can be repaired using either open surgery or minimally invasive surgery (i.e. laparoscopic or robot-assisted).
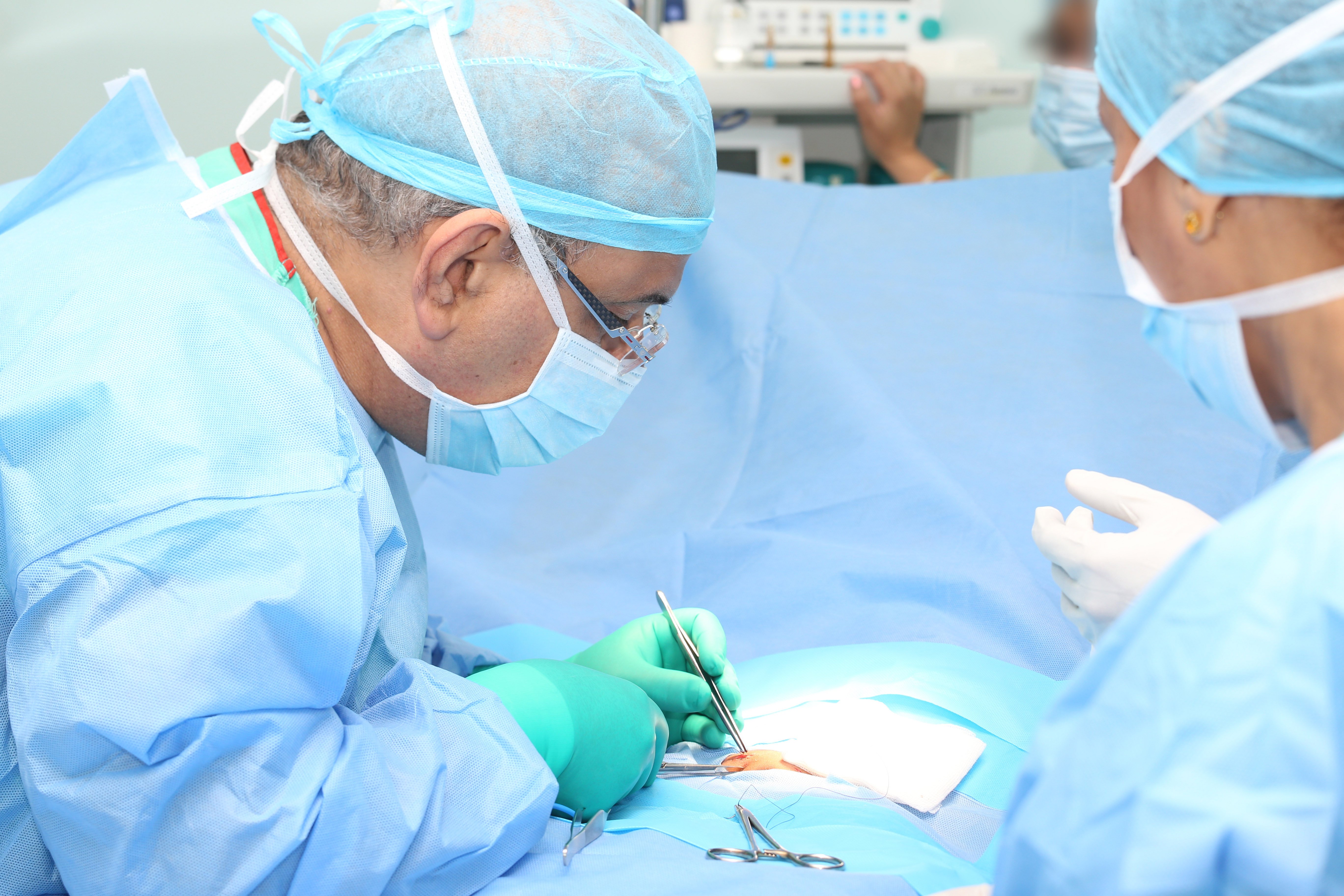 Open Surgery
Open Surgery
The surgeon makes an incision with a scalpel and uses handheld instruments to navigate anatomy and repair the hernia.
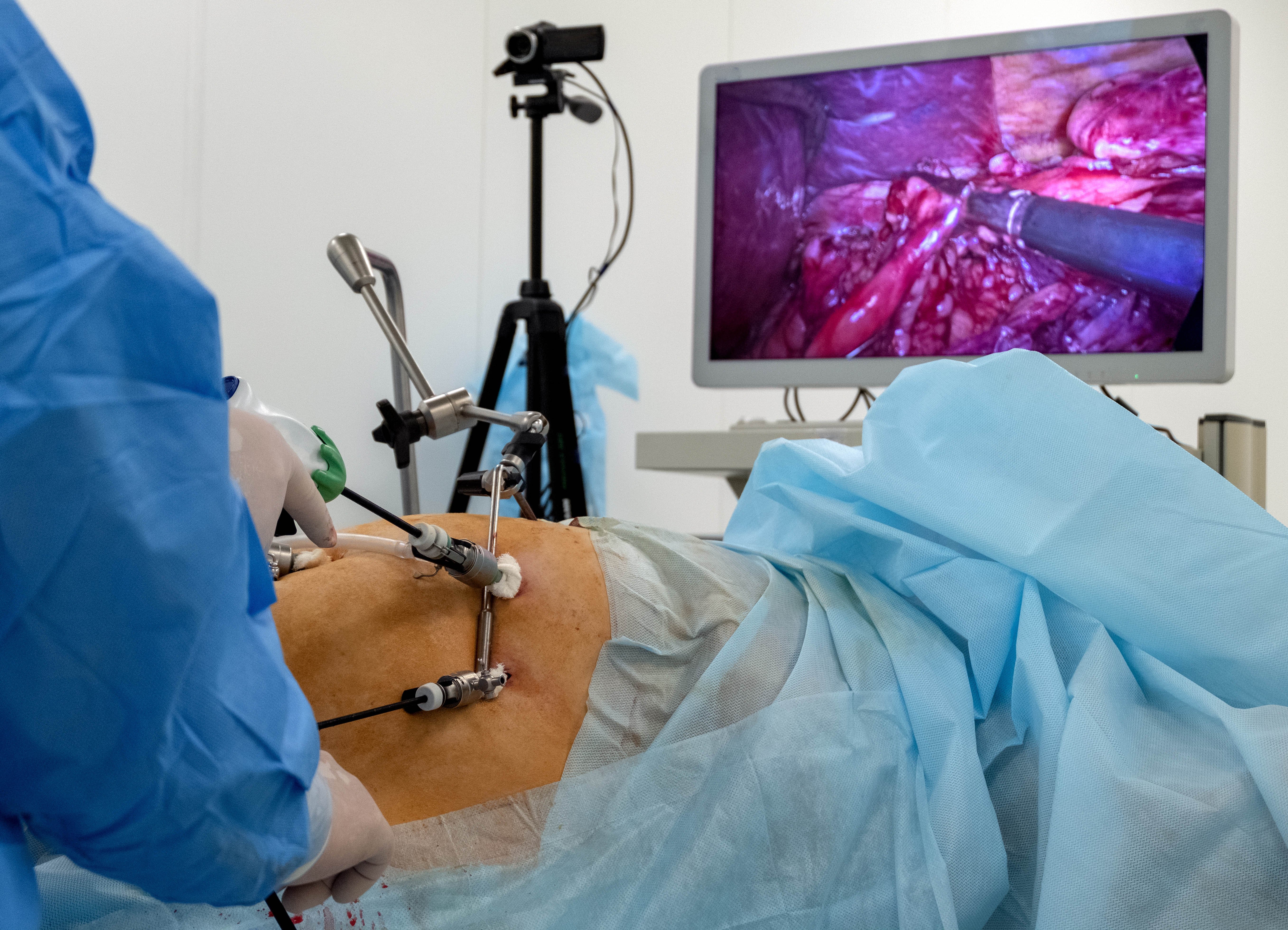 Laparoscopic Surgery
Laparoscopic Surgery
A few small incisions are made to place ports which are used to introduce instruments and a camera, providing the surgeon with enhanced visibility to repair the hernia.
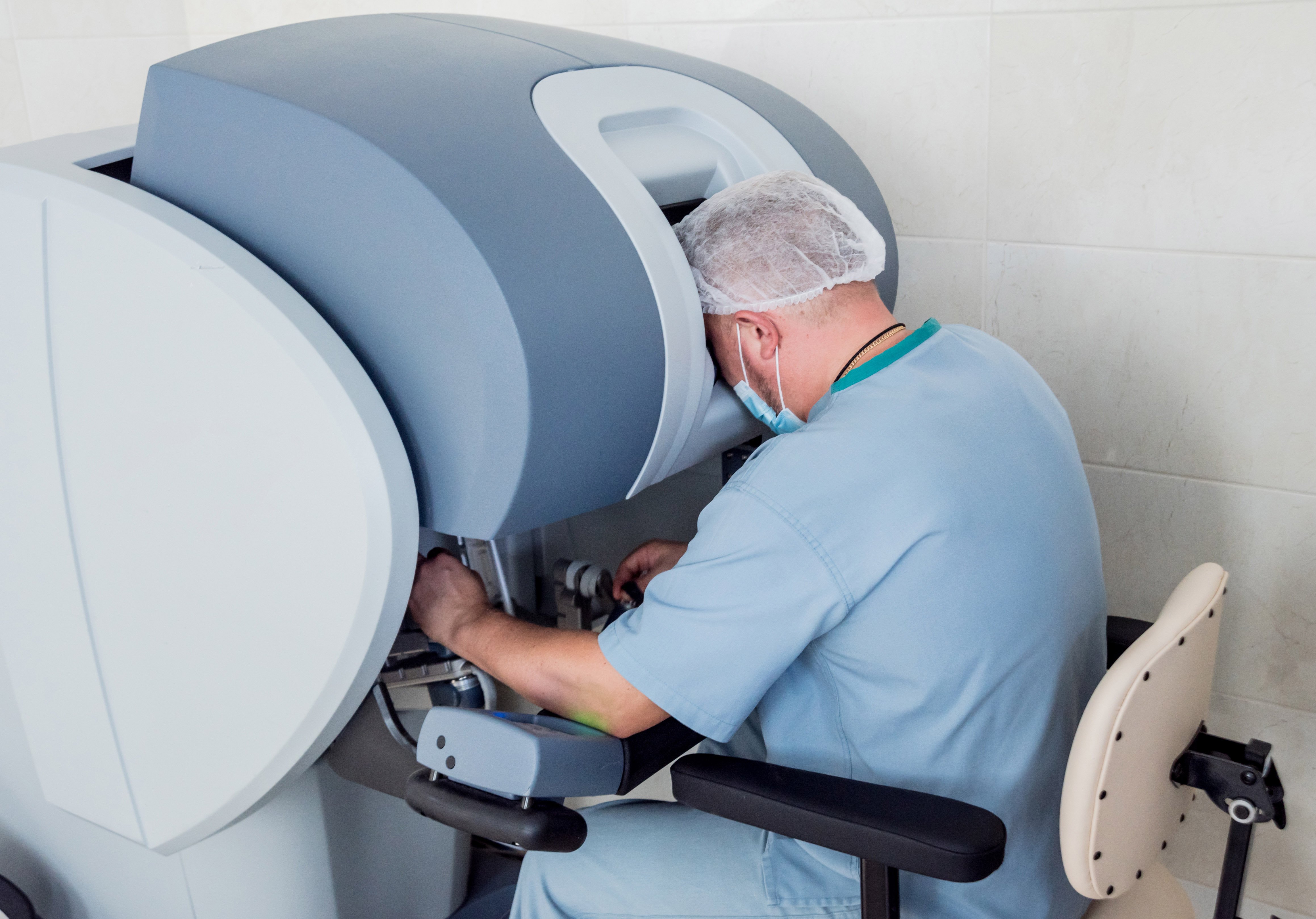 Robot-Assisted Surgery
Robot-Assisted Surgery
Similar to laparoscopic surgery with small incisions and ports, the surgeon repairs the hernia by controlling fully articulating robotic instruments from a console that displays a 3D view of the patient’s anatomy.
What hernia repair surgery is right for me?
Use this framework to help evaluate your options.
There are many interconnected factors such as anatomical location of the hernia, defect size, medical history, patient preference, surgeon experience, repair material availability, insurance coverage, and procedural cost that must be considered to determine the optimal approach to repair the hernia.
While the decision may seem complex, your surgeon will help you determine a care plan.
No two hernias are the same, and everybody's regenerative healing capabilities vary and can be impacted by comorbidities, genetics, diet, and lifestyle.
The amount of foreign material introduced and left behind triggers an inflammatory response, which is an essential part of the natural healing process.3 A prolonged response may lead the body to initiate a defense mechanism that interrupts the regeneration of new tissue, increasing the likelihood of scar tissue formation and potentially leading to recurrence and additional complications.
When considering a surgeon, specialty, years of experience, and bedside manner are important.
Thanks to telehealth, many patients are able to consult with a surgeon to identify fit and only need to travel for the procedure.
It's important to find a surgeon who continues to develop their surgical skills so they can confidently offer the latest innovations designed to improve outcomes.
Find out the surgeon’s preferred surgical approach for treating similar hernias. Often times the “best” hernia repair is the one the surgeon performs the most.
Not all surgeons will have access to a robot and if they do, don't be afraid to ask how many procedures they have performed.
Most importantly, find a surgeon you're comfortable with and have confidence in. If you have reservations, it may be worthwhile to get a second opinion.
A misconception many patients have is that a 'no mesh' hernia repair eliminates the risk of complications from foreign bodies. To repair the tissue defect without using mesh, materials such as suture are utilized, which are often the same absorbable and permanent polymeric materials used to manufacture hernia mesh.
There are over 150 types of hernia mesh available on the market, which include synthetic, absorbable synthetic, biologic, and hybrids, made of a combination of synthetic and biologic materials.4
Be sure to ask about clinical evidence for any implant or repair material that may be used. Published, peer-reviewed safety and outcomes data can help you and your doctor make an appropriate decision.
I don’t want hernia mesh – what other options do I have?
The idea of a mesh implant may trigger fear and anxiety. As very few patients are candidates for a 'no mesh' procedure, it’s important you understand the current clinical evidence and discuss the pros and cons of all available repair options with your surgeon.
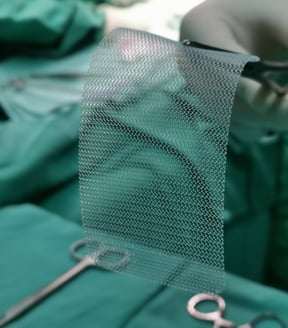
Prepping for Hernia Surgery
Whether this is your first hernia, or you’ve had complications requiring additional procedures, it’s important to work with your healthcare provider to define a plan which is designed to optimize the best potential surgical outcome and post-op recovery.

The areas of focus include:
Hernia Surgery Recovery Guide
Take it slow, with the goal of trying to get better each week. Below is a high-level overview of what you can likely expect with a routine hernia repair. Individual results will vary. Please discuss your recovery timeline with your healthcare provider.
SECTION TIMELINE - TITLE
Description. Lorem ipsum dolor sit amet, consetetur sadipscing elitr, sed diam nonumy eirmod tempor invidunt ut labore et
YEAR - ENTRY TITLE
Description. Lorem ipsum dolor sit amet, consetetur sadipscing elitr, sed diam nonumy eirmod tempor invidunt ut labore et
-
Week 1 - Use Comfort as Your Guide
You will likely have discomfort and swelling the day after the procedure, especially when changing positions. Take it slow and ask your doctor what pain management regimen they recommend.
If you are sent home with a drain or VAC, please follow your discharge instructions from the hospital.
Swelling at or near the surgical site will likely continue for a few days which is normal. However, contact your physician with any concerns about swelling.
-
Week 2 - Start to Move, Stop if You Feel Pain or Discomfort
At this point, it’s good to get moving, but you don’t want to increase abdominal pressure or strain the muscles.
Avoid activities like yoga or Pilates as tensing up abdominals increases pressure.
If you are cleared by your doctor, start with a taking a walk. As you build up stamina, it’s okay to get on a treadmill, elliptical, or stationary bike.
-
Week 3 and 4 - Slowly Returning to Normal
This may be the time you start to return to work and resume normal daily activities. Your abdomen may be ready to experience light twisting and turning.
At your post-op visit, your doctor may also clear you to resume light lifting at the gym or at work. Don't resume any activities without clearance from your treating physician.
-
One Month Post Surgery
Barring any setbacks, your doctor should clear you to return to normal activities. Your abdominal muscles should be healed enough to be able to handle sudden movements like taking your dog for a walk.
For complex abdominal wall surgery, recovery can take up to three months. Your doctor will work with you to develop a recovery game plan.
Post Surgery FAQs
Rather than deal with the anxiety and frustration that comes from asking search engines or social media for medical advice, a collection of general surgeons provide answers to the most frequently asked questions by hernia patients after their surgery.
Week two is likely when your doctor will recommend light physical activity such as walking or riding a stationary bike. Yoga or pilates is not recommended as you want to decrease intra-abdominal pressure.
Don’t lift heavy objects as like deadlifts as it may create significant abdominal pressure.
At week three or four you may be cleared to experience light twisting and turning motions.
It is highly recommended to wait until the swelling goes down. Depending on the repair material, surgical technique, and your healing progress, it may be possible to have sex 5-7 days after surgery. Like all other post-op activities, you should consult with your treating physician.
While you may experience swelling, bruising, and minor pain after surgery, please call your doctor if you experience fever, shooting pain, and / or no bowel movement after three days.
Every patient will have a slightly different response to the surgery. While some may feel a tugging or pulling sensation near the incision for a few days post-op when they suddenly switch positions, others may notice the feeling weeks or months later. If the sensation is causing persistent discomfort that negatively impacts your quality of life, please contact your doctor.
You may have a drain inserted by your incision, which is designed to help remove excess fluid to aid the healing process and help minimize complications like an infection. Depending on the complexity of your procedure, the drain may stay in for a few days. You will receive detailed instructions for drain care at the time of your discharge from the hospital.
It depends on the location of your hernia and your incision sites. It’s advised to wear your binder as much as possible the first few weeks post-op. Some patients feel comfortable sleeping in a reclining chair for a few days after surgery as that reduces the number of times you have to sit up. Side sleepers may need to use a pillow between your legs to provide additional support.
For patients with both GERD and sleep apnea, you may be at additional risk for a hiatal hernia.5 Consider consulting a bariatric surgeon.
As it’s important to reduce intra-abdominal pressure after surgery to help the healing process, consider a bland diet for the first week. It is common to temporarily lose your appetite after hernia surgery.
Depending on your job and the type of procedure you had, your doctor may clear you to return to work 3-5 days post-op. It’s important to listen to your body and don’t exert yourself too much.
It's very common to experience mild to moderate pain after hernia surgery which typically lasts about a week and can be managed with over-the-counter pain medications. For most patients, your second day post-op may be the most painful.
Up to 16% of people experience chronic pain following the repair of a groin hernia.6 It’s important to speak to your doctor if the pain is negatively impacting your quality of life two to three months after surgery.
The number one sign to look for is bulging, swelling, or fullness at the repair site as that may indicate fluid buildup. In certain cases, a drain may be inserted to reduce the amount of fluid, which can help prevent infection and further downstream complications like a revision surgery.
If you experience any one of these symptoms or have any concerns how your hernia repair is progressing, contact your doctor to determine the appropriate treatment.
Depending on how your body handles fluid, your weight may fluctuate slightly after hernia surgery.
You may experience a decrease in appetite that could last a few days. Depending on your BMI, your doctor may recommend a diet and exercise regimen which is important for minimizing the chance of hernia recurrence.
If you are experiencing persistent flu like symptoms such as a high fever, nausea, and vomiting in addition to difficulty passing gas or stool you may be showing symptoms of a mesh rejection. Other symptoms include redness around the repair site and abdominal stiffness or a hard lump. Please seek medical attention immediately.
References:
1. Fitzgibbons RJ Jr, Ramanan B, Arya S, et al. Long-term results of a randomized controlled trial of a nonoperative strategy (watchful waiting) for men with minimally symptomatic inguinal hernias. Ann Surg. 2013;258(3):508-515. doi:10.1097/SLA.0b013e3182a19725
2. Retrieved from https://www.fda.gov/medical-devices/implants-and-prosthetics/hernia-surgical-mesh-implants
3. Kokotovic, D., Burcharth, J., Helgstrand, F. et al. Systemic inflammatory response after hernia repair: a systematic review. Langenbecks Arch Surg 402, 1023–1037 (2017). https://doi.org/10.1007/s00423-017-1618-1
4. Russo Serafini, Mairim, et al. "The Patenting and Technological Trends in Hernia Mesh Implants." Tissue Engineering Part B: Reviews 27.1 (2021): 48-73.
5. Peter J. Kahrilas, Obstructive Sleep Apnea and Reflux Disease: Bedfellows at Best, Chest, Volume 137, Issue 4, 2010, Pages 747-748, ISSN 0012-3692, https://doi.org/10.1378/chest.09-2496.
6. Andresen K, Rosenberg J. Management of chronic pain after hernia repair. J Pain Res. 2018;11:675-681. Published 2018 Apr 5. doi:10.2147/JPR.S127820

